Knee Pain – Ligament Injuries
 Ligaments of the Knee
Ligaments of the Knee
A ligament is a tough band of white, fibrous, slightly elastic tissue that forms an essential part of skeletal joints, and acts to bind bones together. Ligaments prevent dislocation, and restrict excessive movement that might cause injury.
There are four main ligaments as well as supporting ligamentous structures that should be addressed for all knee problems.
The Iliotibial Band (ITB) is a wide, flat ligamentous structure that originates at the iliac crest and inserts onto the outer aspect of the tibia, just below the knee. The ITB serves as a ligamentous connection between the femur (at the lateral femoral epicondyle) and the lateral tibia (at Gerdy’s Tubercle). Since the ITB is not attached to bone (as it passes between the femur and the tibia), it is able to move forward and backward with each knee flexion and extension.
Anterior cruciate ligament (ACL) is often injured by a sudden rotational motion of the knee. Cruciate means ‘crossed’. The anterior and posterior ligaments cross each other in the middle of the knee joint. The ACL attaches to the front of your shin bone (the anterior intercondylar area of the tibia) and acts to restrict anterior motion (prevents forward displacement) of the tibia (shin bone) on the femur (leg bone). The ACL works with the muscles in the back of the knee to prevent hyperextension of the knee.
Posterior cruciate ligament (PCL) is often injured by the effects of a direct impact such as might occur in a sporting event, or a motor vehicle impact. This ligament attaches to the back of your shin bone (the posterior intercondylar area of tibia) and works to restrict posterior motion (prevents backward displacement) of the tibia (shin bone) on the femur (leg bone). Squatting actions cause increased stress on the PCL.
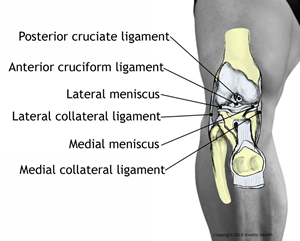 Medial collateral ligament (MCL) is often injured by some type of trauma to the outside of the knee. MCL injuries are common in hockey, football, rugby, or other high-contact sports. The MCL runs from the inside of the leg bone (femur) to the inside of your shin bone (upper medial shaft of the femur). This ligament stabilizes the inside (medial side) of the knee joint.
Medial collateral ligament (MCL) is often injured by some type of trauma to the outside of the knee. MCL injuries are common in hockey, football, rugby, or other high-contact sports. The MCL runs from the inside of the leg bone (femur) to the inside of your shin bone (upper medial shaft of the femur). This ligament stabilizes the inside (medial side) of the knee joint.
Lateral collateral ligament (LCL) can be injured by an impact to the inside of the knee. The LCL runs from the outside of the leg bone (femur) to the outer bone just below your knee (head of the fibula). This ligament stabilizes the outside (lateral side) of the knee joint.
All these ligaments work synergistically and independently to stabilize the knee without the active participation of the surrounding muscles. For example, when your knee is extended, all these ligaments tighten up. However, when your knee is slightly bent, numerous other muscles come into play to stabilize the knee.
Your body maintains a fine balance of structural activity when moving from passive ligament stabilization to active muscle control. Restrictions in either ligament motion or muscle contraction can create a weak link in the kinetic chain. These weak links creates friction-related syndromes, increases inflammation, and causes development of scar tissue or ad
hesions.
Levels of Ligamentous Injuries
 The type of traditional treatment that is prescribed for ligamentous injuries is dependent upon the degree of injury and the type of activities the patient will be involved in after the injury. Ligamentous injuries are classified into the following major grades:
The type of traditional treatment that is prescribed for ligamentous injuries is dependent upon the degree of injury and the type of activities the patient will be involved in after the injury. Ligamentous injuries are classified into the following major grades:
- Grade 1 describes microscopic tears of the ligament. Grade 1 injuries typically respond well to soft-tissue treatments and rehabilitative therapies.
- Grade 2 describes partial tears of the ligament. Grade 2 injuries also respond well to soft-tissue treatments, and generally do not require surgical intervention if treated correctly.
- Grade 3 describes complete tears or rupture of the ligament. Grade 3 injuries require surgical intervention to correct the problem.
Upon the initial onset of an injury to the ligaments, it is important to:
- Rest – Avoid putting excess stress on the knee. In some cases, if the injury is severe, crutches may be advisable.
- Ice – Use ice on the knee for 20-30 minutes, every 2-3 hours, until the swelling is reduced.
- Elevate – Elevate your knee to help reduce inflammation. Place a rolled up blanket or pillow under your knee.
- Compress – Apply an elastic tensor bandage to your knee to reduce swelling.
Manual Therapy for an Ligament Injuries Manual therapy can make a huge difference in the recovery and prevention of an ankle sprain. By manual therapy, I am referring to techniques such as Active Release, Graston Technique, Massage Therapy, Fascial Manipulation, Manual Manipulation, and other manual procedures. In my opinion, these procedures are essential in the rehabilitation of any knee injury since they all act to break down and prevent scar tissue formation.
Manual therapy can make a huge difference in the recovery and prevention of an ankle sprain. By manual therapy, I am referring to techniques such as Active Release, Graston Technique, Massage Therapy, Fascial Manipulation, Manual Manipulation, and other manual procedures. In my opinion, these procedures are essential in the rehabilitation of any knee injury since they all act to break down and prevent scar tissue formation.
Manual therapy also speeds healing by increasing blood supply, oxygen, essential nutrients, and displace waste products that accumulate after an injury. This is especially important in treating ligaments because they generally have a very poor blood supply to begin with.
Manual therapy can also help prevent these conditions from ever arising in the first place. It does this by improving the quality of all the soft-tissues affecting the knee. By ‘quality’, I am referring to your muscle’s ability to store and release energy; much like an elastic cord that stretches and releases efficiently until multiple knots are tied into it. Muscles, much like elastic cords, function extremely well until they build up adhesions from repetitive motion, injury, or muscle imbalances.
The good news is that when these adhesions are removed, your muscles can absorb more shock, become stronger, and improve their reaction times.
Again, as with all injuries, the treatments must be accompanied by the appropriate exercise routines to rehabilitate and restore your tissue’s kinetic chains.
If you would like more information or to purchase our books please go to www.releaseyourbody.com.
If you would like information about our clinic in Calgary Alberta please go to www.kinetichealth.ca.
(COPYRIGHT KINETIC HEALTH 2012 – ALL RIGHTS RESERVED)

Leave a Reply