Resolving Dance Injuries
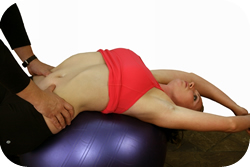 “Ballet ranks with football as the most demanding of all physical activities and sports”.
“Ballet ranks with football as the most demanding of all physical activities and sports”.
- Since 1978 – 3000 articles have been published on dance injuries.
- Between 75-97 % annual incidence of injury reported among professional dancers.
- 80% of dancer have a major injury during their career.
- 93% of dance teachers become teachers because of injury. These injuries often go untreated (often due to financial constraints)
- 65% of injuries dance are overuse 35% are acute or traumatic injuries Byhring 2002.
- Only 2% of dance injuries need surgery – 98% can be treated with conservative therapy (Physiotherapy, Chiropractic, Active Release, Graston).
- The average dancer does 200 one leg landing jumps per class – These jumps can produce a force equivalent to 12 times the dancers body weight.
- There are two common four letter swear words in dance “ Food” and “Rest”.
A high level of fatigue is common in most dancers – Many of the injuries that occur, happen during times of increased fatigue. There are three main deleterious effects of fatigue, that are very well documented: decrease proprioception, impaired balance, decrease joint stability – Altered muscle recruitment patterns
- Burnout is very common in dancers, which causes: decreased strength, decreased coordination, decreased cognitive function, decreased immune function
- Burn out often comes from prolonged stress – dancers are often perfectionists (unrealistic standards, self critical, full of self doubt, often have perfectionist parents).
 Three Stages of Stress
Three Stages of Stress
Stage One
- Increased heart/respiration rate (increased blood pressure)
- Stomach problems (blood flow is being moves from GI tract to Skeletal muscles).
- Increased muscles tension (decreased flexibility, coordination, muscle pain common, headaches).
- Decreased cognitive function
Stage Two
- Level of fatigue increases (affects mental attitude – avoidance strategies common, avoidance of tasks etc, increased procrastination).
- Overall lack of motivation
- Insomnia common (associated weight gain – increased stress hormones, alteration in eating patterns)
Stage Three
- Depression
- Chronic fatigue (mental and/or physical)
- Increase in health problems
- Avoidance of all activities
(Dr. Hans Selye’s “General Adaptation Syndrome).
Prevention of burnout in dancers
- Balancing activity with rest
- Periodization training (Professional dancers do not do what other athletic disciplines do, they often dance at same level throughout the year).
- Sleep
- Good dietary habits – Dancers are known for the three nutritional C’s – Coffee, Cigarettes, and Candy
Medial Ankle Pain – Dancer’s Tendonitis
 An injury to the Flexor Hallucis Longus (FHL) tendon causes medial ankle pain or pain on the bottom of the foot. FHL injury is a condition that is often overlooked or misdiagnosed. This injury affects dancers, runners, soccer players, and any other athlete who performs repeated, propulsive forces, or jumping. Injury of theFlexor Halicus Longus muscle is sometimes called “Dancer’s tendonitis” but it is not limited to just dancers.
An injury to the Flexor Hallucis Longus (FHL) tendon causes medial ankle pain or pain on the bottom of the foot. FHL injury is a condition that is often overlooked or misdiagnosed. This injury affects dancers, runners, soccer players, and any other athlete who performs repeated, propulsive forces, or jumping. Injury of theFlexor Halicus Longus muscle is sometimes called “Dancer’s tendonitis” but it is not limited to just dancers.
The Flexor Hallucis Longus (FHL) muscle allows you to point your big toe (plantar-flexing your big toe) and stabilizes the Subtaler Joint. The Subtaler Joint is located between two bones in your ankle – the Talusand the Calcaneus. The Subtaler Joint allows movement of the heel toward the medial plane (inversion) as well as movement of the heel towards the lateral plane (eversion).
Anatomy/Biomechanics of Medial Ankle Pain
The Flexor Hallucis Longus muscle is located deep under your calf muscles (the most lateral muscle of the deep compartment). The FHL originates on the lateral lower leg (distal 2/3 of Fibula). It then travels at an oblique angle (crosses the posterior surface of Tibia) down towards the medial ankle (posterior surface of Talus) and travels under a section of the heel bone (Sustentaculum Tali of Calcaneus). The FHL then passes under the sole of the foot (between the two heads of the FHB) and inserts into the base of the big toe (base of the Distal Phalanx of Hallax).
As mentioned the FHL Tendon curves around a structure called the Sustentaculum Tali. TheSustentaculum Tali is a bony section on the inside of the heel bone (Calcaneus). This is often a site of friction and irritation for the FHL tendon. The FHL tendon also travels between the twoSesamoid bones just behind the big toe (Metatarso-Phalangeal Joint). The sheath that surrounds the FHL tendon is often irritated.
Causes and Presentation of Medial Ankle Pain
 The repetitive motion of pushing-off with your foot (plantar flexion) during dance, running, soccer, and jumping can cause injury to the FHL.
The repetitive motion of pushing-off with your foot (plantar flexion) during dance, running, soccer, and jumping can cause injury to the FHL.
Injury to the FHL tendon and muscle can present in a variety of ways – sometimes involving inflammation and sometimes not. Injury to the tendon without inflammation is refer to as a “Tendinopathy”. Tendinopathy refers to a degenerative lesion in the tendon without affecting the tendon sheath that surrounds the tendon.
When FHL inflammation (tendonitis) is present in the foot, it usually occurs in one of the following three locations.
- Inside of the ankle (fibro-osseous tunnel along the Posteromedial Ankle).
- At the “Knot of Henry” – a section just behind the big toe (first metatarsal) where the FDL muscle crosses the FHL tendon.
- Just behind the big toe by the Sesamoids bone.
- A Sesamoid bone holds its tendon away from the center of the joint and acts to increase mechanical force.
When the FHL tendon becomes nodular, a condition called Hallux Saltans can develop. Hallux Saltans is similar to trigger finger in the hand, except it occurs in the big toe. Triggering of the toe occurs when the nodular thickening of the tendon snaps through the fibro-osseous tunnel. This causes a jerking motion, much like a trigger finger.
If not addressed Hallux Saltans can contribute to the progression of an additional condition called Hallux Rigidus. Hallux Rigidus means “stiff great toe”. Hallux Rigidus is the second most common disorder of the first MTP joint. The most common injury is a bunion – otherwise known as Hallux Valgus.
Special Considerations For The Dancer
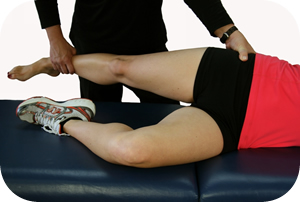 Injury to the FHL in dancers is often caused by the repetitive motion of changing position from a plié position to a relevé position. This action produces a force that is 10 times the dancer’s body weight.
Injury to the FHL in dancers is often caused by the repetitive motion of changing position from a plié position to a relevé position. This action produces a force that is 10 times the dancer’s body weight.
Ideally, for greater stability and increased propulsion, the foot should be in a supinated position at the heel during push-off. For a dancer, any action that causes a reduction in plantar flexionmotion can create an FHL injury. Biomechanically, a lack of plantar flexion leads to a prolonged pronation position of the foot when pushing off in the Propulsion Phase.
In dancers, the FHL tendon is often compressed while performing a relevé position and is over-stretched while performing a plié postion. In such a case, the dancer will feel posterior medial ankle pain when performing the plié.
Diagnosis and Imaging – FHL Injury
X-rays for this condition are not very specific. X-Rays are good for ruling out fractures (Calcaneus, Distal Medial Malleolus, or Os Trigonum) that may cause an impingement of the FHL tendon. It is important to note that X-Rays will not provide a definitive diagnosis of FHL injuries.
A good history is much more definitive, especially when accompanied by a full physical examination and an MRI. MRI imaging is an excellent resource for showing damage to tissue fibers, inflammation, and swelling (edema).
If the MRI is not available or is too expensive, a CT scan (Computed Tomography) can prove to be a useful alternative.
Treatment
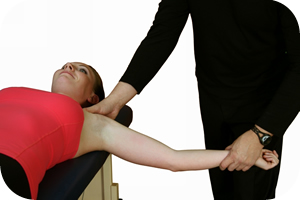 In most cases, FHL syndrome (involving partial tears, tendinosis, or inflammatory conditions) responds well to conservative care. However, a complete tear of the FHL tendon may require corrective surgery since serious cases of FHL injury could end an athlete’s career.
In most cases, FHL syndrome (involving partial tears, tendinosis, or inflammatory conditions) responds well to conservative care. However, a complete tear of the FHL tendon may require corrective surgery since serious cases of FHL injury could end an athlete’s career.
Conservative care includes:
- Ice or heat depending on stage and type of injury (inflammation or not). See our Icing andHeating blog.
- Reduction in activity. Usually, some modification in all activities is necessary.
- Supports (crutches or walker boot) can be beneficial.
- Taping – Kinesio Taping. At Kinetic Health we use SpiderTech Kineso-taping.
- Soft-tissue and joint mobilization (Active Release, Graston Techniques, Massage, and Fascial Manipulation).
- Inflammatory strategy implementation (medication for no longer than seven days). See ourblog about Reducing Inflammation.
- Exercises for increased strength, flexibility and balance. Go to www.releaseyourbody.comfor exercises you can use to treat this condition.
- Biomechanical corrections (footwear or Orthotics) .
- A gradual return to activities.
