Resolving Frozen Shoulder
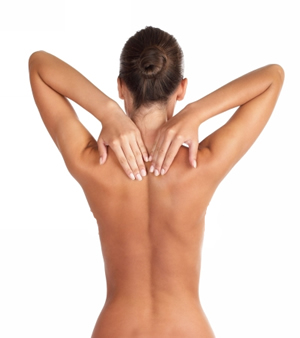 Frozen Shoulder, or adhesive capsulitis, is a very stubborn, debilitating, and restrictive condition which affects all activities of daily living, and is characterized by:
Frozen Shoulder, or adhesive capsulitis, is a very stubborn, debilitating, and restrictive condition which affects all activities of daily living, and is characterized by:
- Severe pain, progressive stiffness, and loss of motion in the shoulder joint.
- Decreased range of motion, with obvious difficulties in raising the arm above the head, across the body, or behind the back.
- Pain that can last from weeks to many months.
- Loss of movement that can last months to years.
Fortunately, you can take steps to control the pain and regain full range of motion. Click on each of the following tabs for more information about how we work with you to heal your injury and the following topics.
- About Your Glenohumeral Shoulder Joint
- Causes of Frozen Shoulder
- Effects of Frozen Shoulder
- Treating Frozen Shoulder
- How ART Helps
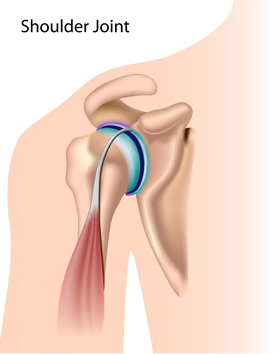
The Glenohumeral (Shoulder) Joint
Your shoulder joint (glenohumeral joint) is a ball and socket joint in which the end of your upper arm (humerus) forms the ball and unites with the socket (glenoid fossa) of the shoulder blade (scapula).
This joint is surrounded by a ligamentous capsule which is full of synovial fluid that lubricates the joint and allows for easy motion. Synovial fluid is a viscous, lubricating fluid which is secreted by the membrane lining the joints and tendon sheaths. The capsule is designed for optimal motion, with numerous folds that allow for movement. The capsule, by itself, is not very strong. However, it is surrounded by the rotator cuff muscles which act as active ligaments and provide stability for the structures of the shoulder.

Frozen Shoulder
Causes of Frozen Shoulder
The actual cause of this condition is unknown, but Frozen Shoulder commonly occurs after:
- Extended periods of immobilization.
- Trauma, injury, or a previous surgery to the shoulder.
- Experiencing conditions such as diabetes, lung disease, heart disease, hyperthyroidism, and Parkinson’s.
Effects of Frozen Shoulder
With Frozen Shoulder, the capsule surrounding the shoulder joint becomes inflamed, thickened, and extremely rigid. This is often accompanied by a decrease in the levels of synovial fluid within the capsule, followed by contraction of the joint capsule.This combination of inflammation and contraction leaves less space for the upper arm bone (humerus) to move around.
The development of Frozen Shoulder is typically divided into three phases, with each phase lasting for several months before change is noticed:
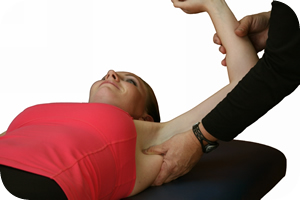
ART Treatment for Frozen Shoulder
Painful Phase (2-9 months): This phase is characterized by pain with any movement and is accompanied by a decrease in the patient’s range of motion.
Frozen Phase (4-12 months): The level of pain decreases, and is accompanied by a substantial decrease in the shoulder’s range of motion. All the activities of daily living become extremely difficult to perform.
Thawing or Recovery Phase (5-26 months): The range of motion will begin to increase and the patient’s pain diminishes.
Treating Frozen Shoulder
There is no doubt that Frozen Shoulder is one of the tougher conditions to treat. The good news is that 80 – 90% of patients suffering from Frozen Shoulder will eventually experience a complete recovery. The bad news, recovery that is based on conventional therapy (muscle relaxants, corticosteroid injections), can take a very long time (twelve to forty-two weeks).
A solution that works!
 Fortunately there are alternatives to these traditional therapies, and that with the right therapy, treatment time can be reduced to between 4 to 10 weeks. I have consistently seen positive results in over 80% of cases treated with a combination of specifically designed Active Release protocols and the correct combination of rehabilitative exercise routines.
Fortunately there are alternatives to these traditional therapies, and that with the right therapy, treatment time can be reduced to between 4 to 10 weeks. I have consistently seen positive results in over 80% of cases treated with a combination of specifically designed Active Release protocols and the correct combination of rehabilitative exercise routines.
At our clinic, we use a treatment protocol that involves:
- Heating the involved shoulder prior to treatment to increase blood circulation and to make the tissue more malleable.
- Administering appropriate ART protocols for Frozen Shoulder.
- Initiating a gentle shoulder exercise routine to mobilize and activate the joint (such as pendulum exercises). See Release Your Pain for examples of some of these exercises.
- Following up with more advanced exercise routines that address range-of-motion, strength, and flexibility as the patient improves. See Release Your Kinetic Chain: Exercises for the Shoulder to Hand for examples of exercises that activate and work the full kinetic chain of the shoulder.
How ART Helps
As we have shown, the shoulder is composed of numerous layers of muscles, tendons, nerves, and other soft tissues. Effective treatment of shoulder problems, or of any soft-tissue injury (ligaments, muscles, blood vessels, fascia, and nerves) requires altering this tissue structure to:
- Break up the restrictive cross-fibre adhesions.
- Restore normal tissue translation and movement.
- Restore strength, flexibility, balance, and stability to the affected soft tissues.
Recommendations during treatment
During the treatment process, we encourage our patients to avoid positions or activities that cause pain. Pushing through the pain can advance the injury, diminish the benefits of the treatment, and result in an increase in treatment time. This caution also applies to the pain that you may experience during exercise.
Note: Pain that is extremely intense, sharp, tearing, or a nerve-type pain is an indication that you are damaging your tissues. You should NOT be feeling this type of pain when exercising. Dull, achy, or compressive pain can occur during light exercise, and is to be expected as you activate and use dormant muscles and structures.
More Information about Frozen Shoulder
Dr. Abelson provides a broad range of information to his patients and the public. They range from published books (eBook and hard-copy), to blogs, exercises YouTube Videos, websites, and articles. Click on the following tabs to access some of his more popular information resources for Frozen Shoulder.
Books to Help you Heal
Both these books provide exercise routines designed to reactivate your kinetic chain and your neuromuscular system. Use these as tools to resolve your Frozen Shoulder.
 Release Your Pain: 2nd Edition
Release Your Pain: 2nd Edition
Dr.Abelson’s international best-seller – Release Your Pain – provides a detailed description about the causes of Frozen Shoulder and other shoulder injuries. It discusses means for resolving this condition, and provides specially selected exercises to help you begin the process of healing from this condition.
Visit our website at www.releaseyourbody.com to purchase your eBook or hard-copy.
 Release Your Kinetic Chain: Exercises for the Shoulder to Hand
Release Your Kinetic Chain: Exercises for the Shoulder to Hand
The phased exercise routines in Exercises for the Shoulder to Hand are designed to build and strengthen the neuromuscular relationships in the structures from your hand to shoulders and core. These exercises are a critical component of any treatment plan for the resolution of Frozen Shoulder. Visit our website at www.releaseyourbody.com to purchase your eBook or hard-copy.
Videos for Frozen Shoulder
The following videos provide extra information about Frozen Shoulder and the kinetic chain, as well as exercises to help resolve this shoulder injury. Click on the left and right arrows to scroll through the videos.
- Shoulder Exercises with Swiss Ball on the Wall
- Click To PlayPlay Video
Ball circles against the wall and Four Cardinal Points both work on proprioception, balance, and coordination of the shoulder and its surrounding muscles.
- Shoulder Injuries: A Kinetic Chain Approach
- Click To PlayPlay Video
Understand how the restrictions in the structures of your shoulder, neck, and back can cause shoulder pain, rotator cuff injuries and a wide array of other problems. Learn how releasing restrictions throughout this kinetic chain can provide a resolution to your shoulder problems.
- Nerve Flossing – Waiters Tip Exercise
- Click To PlayPlay Video
This exercise will help you floss the nerves from your neck, shoulder, elbow, and wrist.
- T’s on the Swiss Ball
- Click To PlayPlay Video
This shoulder exercise is great for training scapular movement after an injury. An essential exercise after a shoulder injury.
- Foam Roller Exercise – The Forearms
- Click To PlayPlay Video
The foam roller is a great tool you use to help resolve Golfers Elbow, or other elbow problems.
Blogs about Frozen Shoulder
Click on the following blog articles for additional information on Frozen Shoulder.
 About Frozen Shoulder
About Frozen Shoulder
With Frozen Shoulder, the capsule surrounding your shoulder joint becomes inflamed, thickened, and extremely rigid. This is often accompanies by a decrease in the levels of synovial fluid within the capsule, followed by contraction of the joint capsule.This combination of inflammation and contraction leaves less space for the upper arm bone (humerus) to move around.
 How Abnormal Motion Patterns Cause Shoulder Injuries
How Abnormal Motion Patterns Cause Shoulder Injuries
Research has shown that extended periods of shoulder instability (glenohumeral instability) can start a cycle of micro-trauma and secondary impingement syndromes which often result in chronic shoulder pain. Practitioners will often find this type of instability during shoulder examinations and translation tests.
 Your Shoulder’s Kinetic Chain
Your Shoulder’s Kinetic Chain
Your shoulder is a truly amazing piece of engineering. When functioning correctly, force and energy are easily transferred from your hips and lower extremity, through your core, and into your shoulders. But, as remarkable as these interconnections are, they can also be the root cause of many chronic dysfunctions. That is why our exercise routines focus on key areas of power transference with a focus on whole-body stability.
For more information about our clinic in Calgary, Alberta, please visit www.kinetichealth.ca.
(COPYRIGHT KINETIC HEALTH 2013 – ALL RIGHTS RESERVED)
